
At the office of The Haddon Dentist, our goal is to preserve natural teeth whenever possible, but we also recognize that removing a tooth is sometimes the most responsible path to long-term oral health. When extractions become necessary, we approach each case with the same care, attention, and precision that guide all of our restorative treatments. Patients can expect a thoughtful evaluation, clear explanations of options, and a plan tailored to their medical history and dental needs.
Deciding on an extraction is never rushed. Our team reviews X-rays and clinical findings, discusses alternatives, and explains how removing a problematic tooth can stop the spread of infection, relieve pain, and protect adjacent teeth. We take time to answer questions so patients understand both the immediate steps of the procedure and the follow-up choices for replacing the missing tooth if that is indicated.
Beyond the technical aspects, we prioritize comfort and dignity throughout the experience. From local anesthesia to, when appropriate, sedation options, the focus is on minimizing discomfort and anxiety so patients can move forward confidently. Our approach is patient-centered: every recommendation balances short-term recovery with long-term function and esthetics.
Primary teeth that won’t fall out or are severely decayed
Sometimes a baby tooth refuses to make room for the permanent tooth beneath it. If the primary tooth is stuck, decayed beyond repair, or fused to bone, removing it can allow the permanent tooth to erupt properly and prevent crowding or misalignment as your child grows.
Permanents that are too damaged by decay to be restored
Tooth decay begins at the enamel, but if left unchecked it can advance into deeper structures and destroy the strength of a tooth. When a tooth has lost so much structure that a filling, crown, or root canal cannot provide a durable outcome, extraction protects your overall oral health and stops further complications.
Severe fractures or cracks that undermine tooth viability
Not all chips and cracks require removal, but when a fracture extends below the gumline or compromises the root, there may be insufficient structure to support a restoration. Extracting a hopelessly fractured tooth prevents infection and prepares the site for future replacement options that restore form and function.
Advanced periodontal disease that destroys supporting tissues
Chronic gum disease can erode the bone and soft tissues that anchor a tooth. As attachment is lost and mobility increases, extraction can become the safest choice to halt progression, reduce sources of infection, and preserve surrounding teeth and bone.
Problematic wisdom teeth
Third molars often lack room to erupt properly, leading to impaction, infection, or damage to adjacent teeth. We evaluate wisdom teeth for risk and function; when they threaten nearby structures or repeatedly cause symptoms, removal can prevent future complications.
Extractions as part of orthodontic planning
In certain cases of crowding or bite correction, removing one or more teeth is a strategic step in an orthodontic plan. Careful coordination with your orthodontist ensures extractions are timed and executed to support predictable tooth movement and a stable bite.
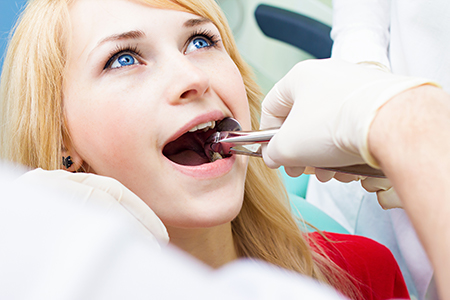
Before any extraction, we complete a thorough assessment that includes a review of your medical history, current medications, and any conditions that could affect healing. Patients should tell us about prescription medications, over-the-counter drugs, and supplements — certain medications can alter bleeding risk or interact with recommended medications. When necessary, we coordinate with your physician to ensure a safe, integrated plan of care.
Imaging is central to modern treatment planning. We use digital radiographs to visualize root anatomy, proximity to important structures, and bone quality so we can select the safest technique. This imaging helps determine whether a straightforward removal is possible or if a surgical approach, sometimes performed by a specialist, is the more appropriate option.
As part of pre-procedure planning, we outline anesthesia and comfort options tailored to the patient’s needs. Local anesthesia effectively numbs the area for most cases; for patients with anxiety or those undergoing more complex extractions, we discuss sedation pathways that maintain safety while improving comfort. Clear pre-operative instructions — such as medication guidance and when to arrive — are provided so the day of the procedure is predictable and calm.
When a tooth is visible and the root anatomy is straightforward, it is often removed in a single visit using a simple extraction technique. After thoroughly numbing the area with local anesthetic, the tooth is gently loosened and removed with forceps. The goal is to preserve as much bone and soft tissue as possible to support healing and future restorative options.
We pay close attention to comfort during every step—patients are monitored, the area is rechecked for complete anesthesia, and breathing or sedation needs are managed. If a patient prefers additional relaxation during the appointment, we will review appropriate sedation choices and ensure monitoring and safety protocols are in place throughout treatment.
Not all extractions can be completed without an incision or access modification. Surgical extraction is used when a tooth is impacted, fractured at the gumline, or fused to bone. This procedure involves a small incision, controlled removal of a limited amount of bone if necessary, and careful sectioning of the tooth to enable atraumatic removal. Doing the work precisely minimizes trauma and supports optimal healing.
Complex cases may be managed by an oral and maxillofacial surgeon, especially when advanced sedation, general anesthesia, or specialized surgical techniques are indicated. Whether performed in our office or by a trusted specialist, the objective is the same: remove the source of pain or disease while protecting nearby structures and laying the groundwork for future restorative care when appropriate.
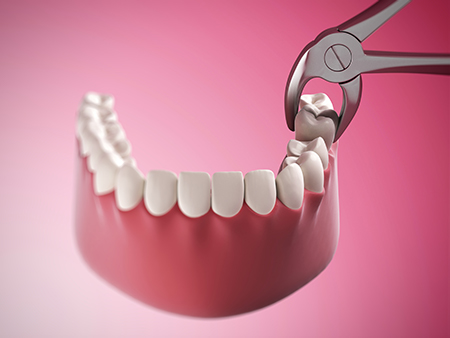
Recovery after an extraction varies with the complexity of the procedure and individual healing responses, but several core principles apply to most patients. Proper clot formation at the extraction site is the first priority; this natural clot protects the bone and nerves while tissue heals. Activities that disturb the clot — such as aggressive rinsing, spitting, or using a straw — should be avoided during the initial 24–48 hours.
Managing swelling and discomfort early helps keep patients comfortable. Applying a cold compress intermittently to the cheek can reduce inflammation during the first day, and following our guidance on pain medication helps control discomfort while avoiding excessive sedation or interactions with other medicines. If antibiotics are prescribed, taking the full course supports infection control when indicated.
Oral hygiene should be gentle but consistent. Brushing nearby teeth carefully, staying hydrated, and introducing a mild saltwater rinse as directed after the first day aid healing and keep the mouth clean. Most patients find that soft foods and avoiding hot or spicy items during the initial days make recovery easier.
Control bleeding with gauze pressure
Bite down on the provided gauze as instructed to help the clot form. Change the gauze after the first hour if necessary, and continue to apply steady pressure rather than repeating periods of heavy spitting. Minor oozing is common for up to 24 hours; contact our office if bleeding appears excessive or continues.
Protect numb tissues
Until sensation returns, be careful not to bite your lips, cheeks, or tongue. Numbness can mask injury, so avoid chewing on the surgical side while the anesthetic persists.
Follow medication instructions
If antibiotics or pain control medications are prescribed, take them exactly as directed. Over-the-counter non-aspirin pain relievers can be effective for many patients; use prescription medications only as instructed and be mindful of interactions with other drugs.
Avoid disturbing the clot
Refrain from rinsing vigorously, drinking through a straw, or smoking for the first week whenever possible. These activities can dislodge the clot and increase the risk of delayed healing or dry socket.
Manage swelling with ice
Apply an ice pack to the cheek in 10-minute intervals during the first 24 hours to help control swelling. After that, warmth can be introduced if swelling persists and the initial inflammation has peaked.
Choose appropriate foods
Stick to soft, cool, and non-spicy foods for the first few days. Keep well hydrated and avoid carbonated or alcoholic beverages during the initial recovery phase.
Maintain gentle oral hygiene
Brush carefully and begin gentle saltwater rinses as recommended to keep the mouth clean without disturbing the surgical site. Follow any suture-care instructions if stitches were placed.
Attend scheduled follow-up
If a follow-up visit is recommended — for suture removal, reassessment of healing, or to plan tooth replacement — keeping that appointment helps ensure the best long-term outcome.
If you notice increasing pain, swelling that worsens after 48–72 hours, persistent bleeding, a bad taste in the mouth, or other unusual symptoms, contact our office so we can evaluate your recovery and intervene if needed.
Extracting a tooth is only one part of a broader plan for oral health. Our practice emphasizes careful decision-making that considers how removing a tooth will affect function, appearance, and future treatment options. When a replacement is advised, we review pathways such as dentures, fixed bridges, and dental implants — each selected to meet the patient’s lifestyle and clinical needs.
Patients find value in a practice that combines technical skill with restorative vision. Whether the plan calls for immediate temporary solutions or staged reconstruction using implant dentistry and precision prosthetics, we design treatment sequences that protect health now and preserve options for the future.
When you need an extraction, you deserve clear communication, experienced care, and a team that coordinates follow-up restorative treatment when appropriate. If you have questions about extractions, recovery, or tooth-replacement options, contact us to learn more and arrange a personalized consultation.

The most common reasons for tooth loss include advanced periodontal disease, extensive tooth decay, and facial trauma. According to statistics, gum disease is responsible for close to 70% of tooth loss in adults. Although less frequent than the preceding three reasons, it should also be noted that specific diseases, drugs, smoking, and poor nutrition contribute to the risk of tooth loss.
The Centers for Disease Control and Prevention report that in the United States, an average of 12 teeth (including the wisdom teeth) are lost by the age of 50. Also, 26% of adults between 65 and 74 years of age have lost all their teeth.
Every patient and every situation is different. However, when a tooth and the surrounding tissues are numbed with a local anesthetic, you should only expect to feel a bit of pressure, but no pain as the tooth is being loosened from the surrounding tissues and extracted. For patients who are apprehensive and for some surgical extractions, our office will discuss our options in dental sedation to provide further relaxation and reduce any sense of discomfort.
While it's normal to feel some tenderness and swelling following an extraction, the degree of these sensations can vary. It mostly depends on the complexity of the extraction and the body's response to the procedure. We'll recommend or prescribe the appropriate pain medication to help ensure your comfort and give you specific instructions for maximum effectiveness and safety.
Typically, the recovery period following a simple extraction is shorter than a surgical extraction. However, a patient's overall health, habits, the size and location of the tooth, and other variables can influence recovery and healing. To speed up the recovery and avoid any complications, patients must follow the given at-home instructions diligently. We'll carefully review what to expect following your procedure and go over your post-op instructions.
Smoking interferes with blood clot formation, which is an essential first step in the healing process. Blood clot formation not only provides a protective layer to cover the underlying exposed bone and nerve endings, but it also supports the growth of new tissue. Cigarette smoke also contains chemical toxins that can disrupt the healing process and lead to problems such as continued inflammation, infection, or dry socket.
In a very small percentage of cases, a condition known as dry socket can develop in the aftermath of a dental extraction. This painful condition can arise when the blood clot in the extraction site doesn't form properly or gets dislodged. With dry socket, you may experience throbbing pain and symptoms such as bad breath and an unpleasant taste in your mouth. As skilled providers of care, our office will provide immediate treatment to alleviate your discomfort and promote healing.
The last teeth in your mouth to develop, wisdom teeth often do not have enough room to fully erupt or may be positioned in the wrong direction. These issues can affect your dental health as well as overall wellbeing. While some individuals never develop all their wisdom teeth, and a few have sufficient space for them, there are many people with partially or fully impacted third molars. Our office will monitor the development, position, and health of your wisdom teeth and will advise you if and when extractions are indicated.
After a tooth is removed, bone-grafting material is sometimes placed in the socket to promote healing and encourage new bone development. This procedure is often performed to support the eventual and successful placement of a dental implant.
At the office of The Haddon Dentist, we strive to make dental care affordable and accessible. Depending on the type or complexity of the extraction and other variables, the cost of the procedure can vary. Based on our diagnostic findings, our office will inform you of the healthiest choices in care, explain the fees, discuss insurance coverage, and explain your payment options.
Many dental plans offer some level of coverage for tooth extractions. We'll advise you if your plan covers the full cost of the procedure and if there is any out-of-pocket expense. Our business office will work with you to maximize your insurance benefits as much as possible while helping you minimize any out-of-pocket expenses.
Persistent pain, swelling, repeated infections, or a tooth that is mobile are common signs that removal may be necessary. Severe decay, fractures that extend below the gumline, and advanced periodontal disease can render a tooth nonviable even when conservative care is attempted. We use clinical examination and digital radiographs to evaluate these findings and determine whether extraction is the safest course.
Decisions are not rushed; we discuss alternatives such as root canal therapy or restoration when feasible and explain risks and benefits. Removing an infected or structurally compromised tooth can protect adjacent teeth and stop ongoing disease. When extraction is indicated, we also review replacement options so you understand the path forward for function and esthetics at the office of The Haddon Dentist.
A simple extraction is performed when a tooth is fully visible in the mouth and the root anatomy is straightforward; it typically involves local anesthesia and gentle elevation and removal with forceps. Surgical extraction is required when a tooth is impacted, fractured at the gumline, or has roots that require sectioning or limited bone removal to extract safely. The goal in either approach is atraumatic technique that preserves bone and soft tissue for healing and future restorative options.
Surgical cases may involve a small incision, removal of minimal bone, and sometimes sutures to close the site and promote predictable healing. Complex surgical extractions or cases requiring advanced sedation are occasionally referred to an oral and maxillofacial surgeon to ensure the safest outcome. Whether simple or surgical, the treatment plan is tailored to your anatomy, medical history, and restorative goals.
Preparation begins with a thorough review of your medical history, current medications, and any conditions that could affect healing or bleeding. We obtain digital radiographs to understand root shape, bone quality, and relationship to nearby structures, and we coordinate with your physician when systemic issues or medication adjustments are necessary. Clear preoperative instructions are provided so you know when to arrive and what to expect on the day of the procedure.
If sedation is planned, we will give specific fasting and escort instructions to ensure safety; for local anesthesia only, eating a normal light meal is usually acceptable unless otherwise directed. Please tell us about prescriptions, over-the-counter drugs, and supplements so we can assess interactions with prescribed medications. Our team will review anesthesia options and any special considerations to make the appointment as calm and predictable as possible.
On the day of the procedure we confirm your medical information, review the plan, and administer local anesthesia to numb the area; sedation options are available for patients who require additional relaxation. For a simple extraction the tooth is gently loosened and removed with forceps, while surgical extractions may require a small incision, sectioning of the tooth, or minimal bone removal to facilitate atraumatic removal. Throughout the appointment we monitor comfort, vitals as needed, and the surgical site to minimize trauma and support healing.
If sutures are placed they are used to help tissue approximation and may be resorbable or removed at a follow-up visit, depending on the technique. After the procedure we will provide written and verbal aftercare instructions and review expected symptoms and recovery timelines. You will receive guidance about eating, activity, medications, and signs that warrant a prompt evaluation.
Proper clot formation is essential for healing, so avoid vigorous rinsing, spitting, or using a straw for the first 24–48 hours and refrain from smoking as it increases the risk of complications. Bite gently on the provided gauze to control bleeding and change it as directed; minor oozing can be normal during the first day. Maintain gentle oral hygiene by brushing nearby teeth carefully and delaying strong rinses until advised.
Use an ice pack intermittently on the cheek during the first 24 hours to reduce swelling, and transition to warm compresses afterward if swelling persists. Follow medication instructions for pain control and take any prescribed antibiotics exactly as directed when indicated. Stick to soft, non-irritating foods and reintroduce your normal diet gradually as comfort allows.
Most extractions heal without issue, but complications such as dry socket, infection, prolonged bleeding, or nerve-related numbness can occur and usually present with increased pain, swelling, fever, or persistent drainage. Dry socket often appears a few days after the extraction and causes a deep, throbbing pain that may radiate to the ear; infection can cause fever, worsening swelling, and a foul taste or odor. Persistent uncontrolled bleeding or signs of systemic illness should prompt immediate attention.
Contact our office if you experience severe pain that is not relieved by prescribed medications, swelling that worsens after 48–72 hours, persistent bleeding, or any new numbness or tingling that does not resolve. Early evaluation allows us to intervene promptly with appropriate treatments, such as topical therapies for dry socket, antibiotics for infection when indicated, or additional measures to control bleeding. We are prepared to guide you through recovery and schedule an in-person assessment if needed.
Removing a tooth can influence adjacent tooth position, bite relationships, and the long-term function of your jaw, so extractions are considered within a broader restorative plan. Space loss or shifting can occur over time if a missing tooth is not replaced, which may complicate future restorative or orthodontic treatments. For many patients, preserving bone and preparing the site for a future implant, bridge, or denture are important parts of the plan discussed before extraction.
Our practice emphasizes coordinated restorative planning so extractions support long-term function and esthetics, whether that involves immediate temporary measures or staged reconstruction. Techniques such as socket preservation can help maintain bone volume to improve outcomes for implants or other restorations. We evaluate each patient’s needs and sequence treatment to protect options for the future and optimize the final result.
Antibiotics are prescribed only when clinical signs of infection are present or when a patient’s medical history indicates an elevated risk for infection; they are not routine for every extraction. If an antibiotic is recommended, it is important to complete the full course as directed to ensure adequate infection control. Overuse of antibiotics is avoided, and decisions are made based on clinical findings and best-practice guidelines.
Pain management typically includes over-the-counter analgesics for many patients, with prescription-strength medications reserved for more complex or uncomfortable cases. Always inform us of all medications and supplements you take so we can avoid interactions and choose safe alternatives. Follow dosing instructions carefully and contact the office if pain is uncontrolled or if you experience unexpected side effects.
No, wisdom teeth are not automatically removed; their management depends on how they erupt, the space available, and whether they cause symptoms or threaten adjacent teeth. Impacted third molars that repeatedly become infected, damage neighboring teeth, or contribute to cysts or decay are commonly recommended for removal. If wisdom teeth are fully erupted, functional, and easily cleaned, they may be monitored rather than extracted.
We evaluate third molars with clinical examination and radiographs to assess impaction, angulation, and proximity to important structures. When removal is recommended, we discuss timing, technique, and whether referral to an oral surgeon is appropriate for complex anatomy or advanced sedation needs. Regular monitoring is an acceptable approach when wisdom teeth are asymptomatic and pose low risk.
Extractions in children are performed with attention to growth, development, and the timing of permanent tooth eruption; common reasons include severe decay, retained primary teeth that block eruption, or infection that threatens overall oral health. Our approach balances preserving space for permanent teeth with removing sources of disease that can harm developing dentition. We explain the rationale for removal and discuss space maintenance or orthodontic coordination when appropriate.
Behavioral guidance and anesthesia choices are tailored to a child’s age, needs, and level of cooperation, with safety as the primary concern. Parents receive clear pre- and post-operative instructions and education on diet, oral hygiene, and signs of complications to watch for during recovery. When indicated, we collaborate with pediatric specialists to ensure the most appropriate and comfortable care for young patients.

The path to a restored, high-functioning smile is a journey of precision, and it begins with a single, focused conversation. We invite you to experience the intersection of clinical mastery and uncompromising luxury at The Haddon Dentist. Whether you are seeking the immediate results of CEREC® same-day crowns, exploring the life-changing benefits of dental implants, or ready to revitalize your aesthetic with professional teeth whitening, we are here to curate a plan tailored exclusively to you. Your time is your most valuable asset, and we cherish the opportunity to provide the elite care you deserve in an environment that respects your comfort and your goals.