Tooth loss can affect more than just your smile — it influences how you chew, speak, and how your face appears over time. Advances in implant dentistry have shifted the focus from temporary fixes to long-term, biologically sound restorations that restore both function and appearance. Implant therapy places a sturdy foundation where a tooth root once lived, creating results that feel and perform like natural teeth for the long term.
Every patient’s situation is unique, and a successful outcome depends on careful assessment and planning. Our approach evaluates your overall oral health, jawbone condition, and lifestyle so we can recommend the most appropriate implant solution. This methodical process reduces surprises during treatment and helps ensure predictable, stable results.

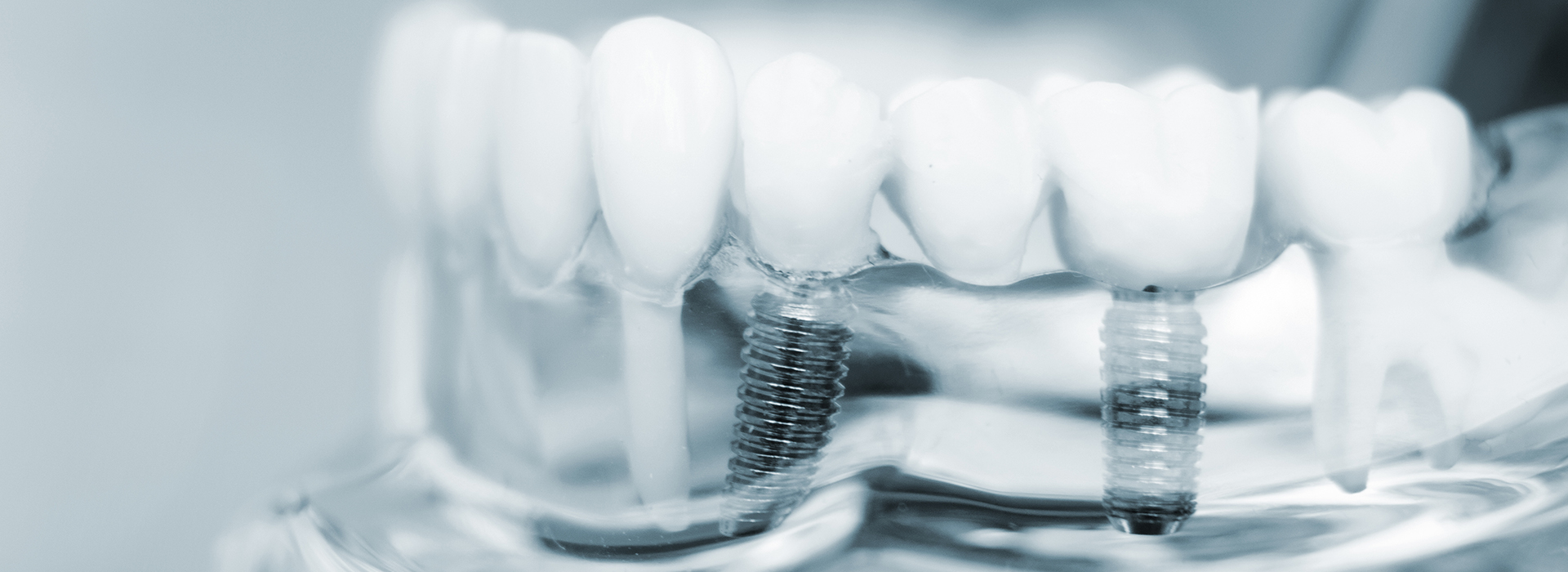
Dental implants are biocompatible posts that are designed to fuse with the jawbone in a process called osseointegration. Once integrated, an implant acts similarly to a natural tooth root, supporting crowns, bridges, or dentures without relying on neighboring teeth for support. This root-like behavior preserves bite mechanics and helps prevent the gradual bone loss that accompanies missing teeth.
Because implants stimulate the underlying bone, they help maintain facial structure and reduce the sunken appearance that sometimes follows tooth loss. For many patients, this translates into improved comfort, clearer speech, and the freedom to enjoy a wider variety of foods without concern for slippage or instability.
Successful implant treatment begins with precise diagnostics. We use advanced imaging and a thorough oral exam to map bone volume, nerve locations, and the relationship between the jaw and adjacent teeth. This information guides implant selection, angulation, and the prosthetic design so your final restoration is both durable and esthetic.
When appropriate, digital planning tools allow us to simulate outcomes and create surgical guides that improve accuracy during placement. These technologies streamline treatment while enhancing predictability — a benefit patients notice in both the short and long term.
Implants provide a flexible foundation for a range of restorations. A single implant topped with a crown replaces one missing tooth without altering adjacent teeth. When several teeth are missing, implants can support a fixed bridge that restores multiple teeth while protecting surrounding natural dentition. For those missing all teeth in an arch, implants can retain or support a full set of prosthetic teeth that look and feel more natural than traditional dentures.
Because implant-supported restorations attach directly to the jaw, they eliminate many of the limitations experienced with removable dentures. Patients commonly report greater confidence while eating, speaking, and smiling when their prosthesis is secured by implants.
Contemporary implant restorations use high-quality materials such as ceramic crowns and precision-milled frameworks that balance strength with natural-looking translucency. The choice of material and prosthetic design is tailored to each patient’s needs, considering bite forces, esthetic goals, and hygiene access. This personalized selection helps ensure the restoration is both attractive and serviceable for years to come.
Your treatment plan will explain the recommended type of restoration and why it best fits your anatomy and expectations. Clear communication about each step reduces uncertainty and helps you make an informed choice about your care.
Implants are often chosen because they restore natural chewing efficiency and stability. They eliminate the worry of slippage that can come with removable dentures and let patients eat a fuller range of textures without special preparation. Many people find that implants immediately improve daily comfort and make social situations less stressful.
Beyond function, implants contribute to oral health by preserving bone. When a tooth is missing, the underlying bone can resorb over time; an implant provides the mechanical stimulation that helps maintain bone volume and supports natural facial contours.
With proper care — regular professional checkups and diligent home hygiene — implants have excellent long-term outcomes. Unlike natural teeth, implant materials do not decay, but the tissues around an implant still require attention. Maintaining healthy gums and monitoring for any changes are essential to preserve implant longevity.
Because implants do not rely on neighboring teeth for support, they can protect adjacent tooth structure from the wear and preparation that conventional bridges sometimes require. This conservative strategy preserves more of your natural dentition while restoring what was lost.
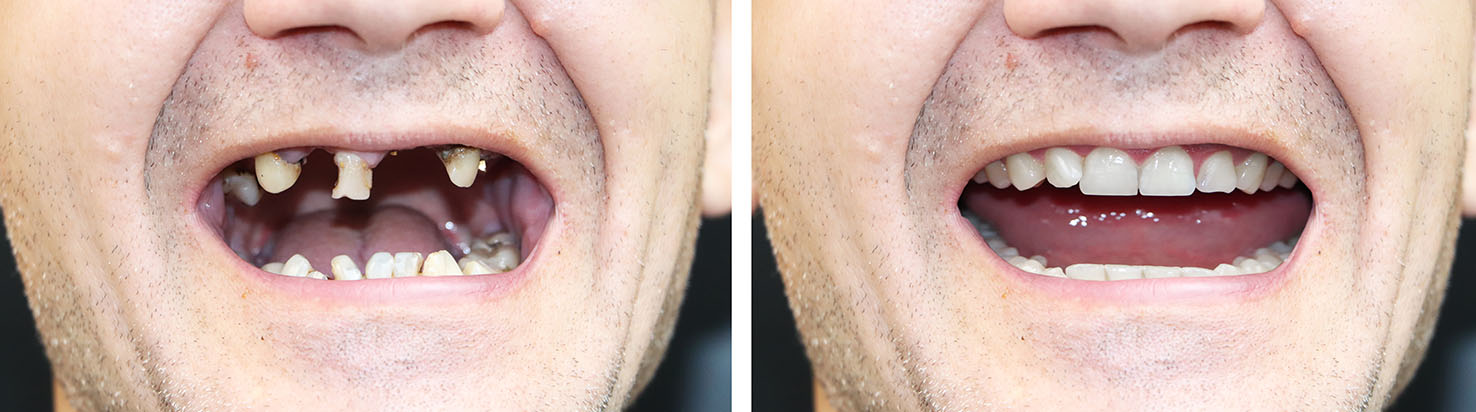
Selecting the best implant option depends on bone quantity, general health, esthetic goals, and daily needs. The treatment process focuses on preserving as much natural structure as possible while delivering a reliable and attractive restoration. We take time to explain the advantages and considerations so you can choose the solution that best fits your life.
Most adults who are in good general health and who have adequate jawbone are candidates for implant therapy. Certain medical conditions and habits can influence timing and planning, so a thorough medical and dental review is part of every consultation. If additional procedures are needed — for example, bone grafting to rebuild lost volume — these options are discussed openly so you understand the recommended sequence.
Implant placement is performed as an outpatient procedure and is typically well tolerated. The surgical approach varies by case complexity: some patients receive a provisional restoration immediately, while others require a healing period to allow the implant to integrate with bone. We discuss anesthesia and comfort options in advance and provide clear pre- and post-operative instructions to support a smooth recovery.
After placement, osseointegration takes place over a few months. During this time, we monitor healing and, when appropriate, proceed with the final restorative phase. Regular follow-up helps ensure the tissues remain healthy and that the final prosthesis meets both functional and esthetic expectations.
In situations where bone volume is insufficient, grafting procedures can rebuild a stable foundation for implants. Grafting materials and techniques are chosen based on the specific anatomy and restorative goals. When grafts are needed, they are integrated into the overall treatment timeline so the final result is both secure and natural in appearance.
Long-term success also depends on routine dental care. Periodic professional assessments and careful home hygiene protect the implant and surrounding tissues, supporting a restoration that serves you well for many years.
Implant dentistry offers dependable, long-lasting ways to restore missing teeth and reclaim oral function. If you’d like to explore whether implants are right for you, the team at The Haddon Dentist can review your situation and outline thoughtful options that align with your goals. Contact us for more information or to arrange a consultation.

If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Dental implants are biocompatible posts, typically made of titanium or titanium alloys, that are placed into the jawbone to serve as stable anchors for replacement teeth. An implant replaces the tooth root and supports an abutment and a custom prosthetic, such as a crown, bridge, or denture. Because the prosthesis is attached to the implant rather than relying on adjacent teeth, the finished restoration functions and feels much like a natural tooth.
Implants restore chewing efficiency and help maintain jawbone volume by transmitting functional forces to the underlying bone. This stimulation reduces the bone loss that commonly follows tooth extraction and helps preserve facial contours over time. The result is a durable, conservative foundation for long-term tooth replacement when proper planning and care are used.
Most healthy adults who have adequate jawbone and healthy oral tissues are potential candidates for dental implants after a thorough evaluation. The candidacy assessment includes a review of medical history, current medications, and lifestyle factors such as tobacco use that can affect healing. Advanced imaging and an intraoral exam determine bone volume, nerve positions, and the relationship of remaining teeth to the planned restoration.
Some medical conditions or medications may influence timing and technique but do not automatically preclude implant therapy when managed appropriately by your dental and medical providers. In cases of insufficient bone or complex anatomy, staged approaches like grafting or guided placement are considered to create a stable foundation. A personalized treatment plan outlines the recommended sequence so patients know what to expect before surgery begins.
Osseointegration is the biological process whereby living bone bonds tightly to the surface of an implant, creating a stable interface similar to a natural tooth root. This direct structural connection is essential because it allows the implant to withstand normal chewing forces without micromotion that could compromise healing. Implant surface design and atraumatic surgical technique both support predictable osseointegration.
Once integration is achieved, the implant provides a reliable support for definitive restorations and helps maintain the mechanical integrity of the dental arch. This stability reduces the risk of prosthetic complications and preserves adjacent tooth structure by eliminating the need to use neighboring teeth as anchors. Long-term success depends on healthy surrounding gum tissue, good oral hygiene, and routine professional monitoring.
Precise diagnostics are the foundation of predictable implant treatment and commonly include three-dimensional CBCT imaging, high-resolution radiographs, and digital intraoral scans when available. These records map bone volume, sinus anatomy, and nerve locations while capturing the existing dentition and occlusion. A detailed clinical evaluation examines gum health, bite relationships, and any factors that could affect surgical or restorative outcomes.
Digital planning software can simulate implant position, prosthetic contours, and final esthetics before surgery, which helps to select optimal implant size and angulation. When indicated, a surgical guide fabricated from the plan improves placement accuracy and reduces intraoperative decision-making. This coordinated workflow aligns surgical and restorative goals so the final prosthesis meets functional and esthetic expectations.
Implant placement is usually performed as an outpatient procedure using local anesthesia and, if desired, additional sedation for patient comfort. The surgeon creates an osteotomy for the implant, inserts the implant body, and places a cover screw or healing abutment; in some cases, a temporary restoration is delivered immediately. Postoperative instructions cover pain control, oral hygiene, diet adjustments, and signs to watch for during the initial healing phase.
Initial soft-tissue healing generally completes within one to two weeks, while osseointegration proceeds over several months depending on clinical factors. Regular follow-up visits allow the clinician to monitor healing and determine the appropriate time for the restorative phase. Most patients experience manageable discomfort that responds to standard analgesics and resolves as tissues recover.
Bone grafting is recommended when existing jawbone volume is insufficient to support an implant of predictable length and diameter. Grafting materials range from the patient’s own bone to processed allograft or xenograft substitutes, and the choice is guided by the clinical situation and restorative needs. In the posterior upper arch, a sinus lift may be performed to elevate the sinus floor and create space for graft material when vertical bone height is limited.
Grafts integrate over several months and become a stable foundation for implant placement either in the same visit or after a healing period, depending on the quality of the grafted site and primary stability needs. Your clinician will explain the timing and sequence so you understand whether placement will be immediate, delayed, or staged. Successful grafting restores the anatomic support needed for durable implant restorations.
Implants can support a range of prosthetic solutions from single-tooth crowns to multiunit bridges and complete-arch fixed restorations supported by four to six implants. A single implant with a crown replaces one tooth without altering adjacent teeth, while strategically placed implants can retain a fixed bridge that restores several missing teeth as a unit. Full-arch fixed solutions provide a non-removable restoration that closely resembles natural teeth in function and appearance.
For patients who prefer a removable option, implant-retained overdentures securely snap onto implants while remaining easy to remove for cleaning. The choice between fixed and removable designs depends on patient preference, anatomy, hygiene access, and functional requirements. A comprehensive evaluation clarifies the advantages and trade-offs so the selected design fulfills both day-to-day needs and long-term goals.
Common restorative materials include high-strength ceramics such as zirconia and lithium disilicate, and metal frameworks often fabricated from titanium or other alloys for strength and precision. All-ceramic crowns and layered ceramic restorations offer excellent esthetics and translucency for anterior teeth, while reinforced frameworks provide durability for posterior prostheses. Material selection balances esthetic demands, functional forces, and maintenance access to create a restoration suited to each situation.
Precision-milled components and modern bonding protocols improve fit and reduce complications related to misfit or wear. The prosthetic design also considers hygiene access, occlusal load distribution, and retrievability for maintenance or repair. Your clinician will recommend materials based on clinical objectives so the final restoration meets expectations for longevity and appearance.
Daily oral hygiene remains essential for implant longevity and includes thorough brushing with a soft or powered toothbrush and cleaning around implant restorations with floss or interdental brushes. Patients should follow a maintenance schedule of professional cleanings and examinations so the dental team can assess tissue health and prosthetic integrity. Avoiding tobacco and addressing systemic health factors, such as uncontrolled diabetes, supports predictable healing and reduces the risk of complications.
During regular visits, clinicians evaluate for signs of peri-implant mucositis or peri-implantitis and provide targeted hygiene instruction or intervention as needed. Early detection and management of soft-tissue changes help preserve bone support and prevent progressive problems. With consistent care and monitoring, implants can deliver durable function for many years.
To start, schedule a consultation so the dental team can review your medical and dental history, perform an oral exam, and obtain any necessary imaging to evaluate bone and anatomic relationships. This initial visit focuses on understanding your goals, explaining treatment options, and outlining the diagnostic and surgical sequence tailored to your needs. Expect a clear plan that describes whether any preparatory procedures, such as grafting, are required and the anticipated timeline for each phase.
The office of The Haddon Dentist coordinates care across diagnostic, surgical, and restorative phases to ensure consistent communication and predictable outcomes. If a referral to a specialist is in your best interest, the practice will explain that recommendation and how it fits into the overall plan. With informed consent and a collaborative approach, patients can move forward confidently toward a durable, well-planned implant restoration.

The path to a restored, high-functioning smile is a journey of precision, and it begins with a single, focused conversation. We invite you to experience the intersection of clinical mastery and uncompromising luxury at The Haddon Dentist. Whether you are seeking the immediate results of CEREC® same-day crowns, exploring the life-changing benefits of dental implants, or ready to revitalize your aesthetic with professional teeth whitening, we are here to curate a plan tailored exclusively to you. Your time is your most valuable asset, and we cherish the opportunity to provide the elite care you deserve in an environment that respects your comfort and your goals.