Missing teeth affect more than appearance; they can change how you speak, what you eat, and how the jaw functions. When a tooth is lost, the surrounding bone and adjacent teeth can shift, leading to changes in bite, uneven wear, and additional tooth loss over time. Implant restorations replace the missing root as well as the visible tooth, helping to preserve facial structure and maintain the alignment and function of the entire dental arch.
Because an implant is anchored in the jaw, it transmits chewing forces through the bone in a way that closely mimics a natural tooth. That functional stability translates into greater comfort while eating and improved confidence when speaking or smiling. For many patients, implant-based restorations feel and behave more like natural teeth than removable options, which reduces the daily reminders of tooth loss.
Beyond function and form, implant restorations also serve long-term oral health. By replacing a missing root, an implant helps preserve local bone volume and provides a stable foundation for restorations that protect neighboring teeth from unnecessary stress. This foundational role makes implants a durable and predictable solution for properly selected patients.
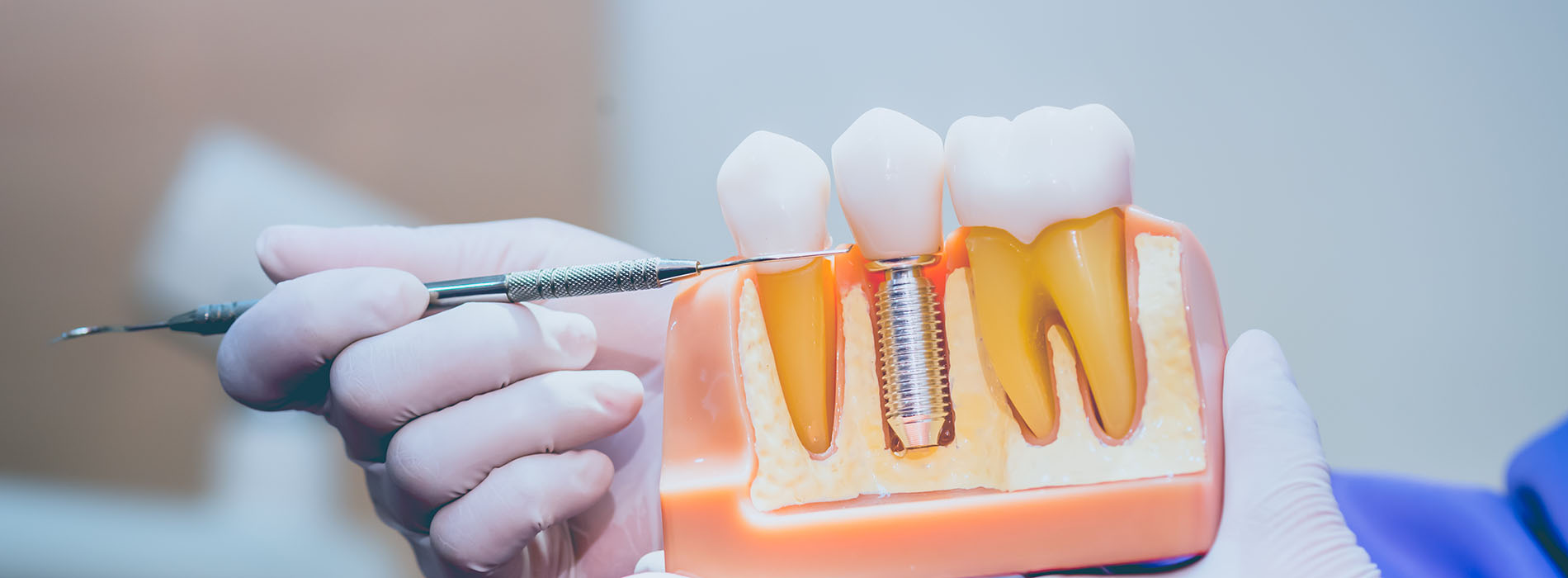
An implant restoration is a multi-component solution designed to replicate the natural tooth from root to crown. The foundation is a small biocompatible post—typically made of titanium or a titanium alloy—surgically placed into the jawbone. Once the post has integrated with the bone, a connecting piece called an abutment is attached to support the visible restoration, which can be a crown, bridge, or an implant-retained denture depending on the case.
The visible portion of the restoration is custom-crafted to match the patient’s teeth in shape, size, and color. Modern restorative materials include high-strength ceramics and porcelain-fused options that provide both resilience and lifelike esthetics. Technological advances in digital scanning and CAD/CAM milling allow precise design and fabrication, resulting in restorations that fit closely to surrounding tissues and deliver a natural appearance.
Throughout the process, clinical decisions focus on long-term stability: implant diameter and length are chosen to suit the available bone, abutment geometry is selected for optimal emergence profile, and the final restoration is contoured to distribute bite forces evenly. This careful planning and sequencing are what distinguish a restoration that functions comfortably for years from one that leads to complications.
Successful implant restorations begin with a thorough clinical evaluation. The dentist assesses dental and medical history, examines the oral tissues, and uses diagnostic imaging to evaluate bone quantity and quality. This information guides decisions about implant location, angulation, and whether additional procedures—such as bone grafting or sinus augmentation—are advisable to create a stable foundation for the implant.
Planning also considers the final restorative goal: a single-tooth crown, a fixed bridge on multiple implants, or an implant-supported overdenture. Working backward from the intended restoration ensures the implant is positioned to support ideal form and function. Digital tools, including 3D imaging and virtual treatment planning, are often used to simulate outcomes and communicate a clear plan to the patient.
Coordination of care is important when multiple specialists are involved. A prosthodontist or restorative dentist oversees the prosthetic design, while an oral surgeon or trained implant dentist may place the implant. The team approach helps ensure each phase—from surgery through restoration—is performed with consistent standards and a shared goal of predictable, esthetic results.
Material selection and restorative design play a central role in how an implant restoration performs and appears. High-quality ceramic materials provide excellent esthetics and wear characteristics, while layered or monolithic options can be chosen based on the patient’s bite, smile line, and functional demands. The restoration is shaped to support healthy gum contours and to make hygiene straightforward for the patient.
Emergence profile and contact points are carefully sculpted to prevent food trapping and to maintain periodontal health. Occlusal considerations—how the teeth meet during chewing and at rest—are addressed to avoid excessive forces on the implant. These design elements reduce the risk of mechanical complications and contribute to the long-term success of the restoration.
When appropriate, digital impressions and milling technologies shorten turnaround time and allow for more precise control of fit and shade. That same digital precision helps the lab or in-office milling unit produce restorations that require minimal adjustment at delivery, improving comfort and minimizing chair time for patients.
Once an implant restoration is in place, routine maintenance and good oral hygiene are essential to protect both the implant and surrounding tissues. Patients are instructed on effective brushing and flossing techniques around implants, and professional cleanings at regular intervals allow the dental team to monitor tissue health, check prosthetic components, and catch early signs of wear or inflammation.
Follow-up visits also include assessments of occlusion and the stability of abutments and screws. Because implants do not have the cushioning of a natural periodontal ligament, improper bite forces or neglect can lead to mechanical or biological complications. Timely adjustments and repairs can address these issues before they compromise the restoration.
Certain lifestyle and health factors can influence outcomes, and the dental team provides personalized guidance to help patients mitigate risk. With attentive home care and routine professional oversight, well-designed implant restorations offer a durable and comfortable solution that supports a confident, functional smile.
Candidacy for implant restorations is based on several factors, including oral health, bone availability, and general health considerations. Many patients who are missing one or more teeth are candidates, but a careful evaluation will determine whether preparatory treatments—such as grafting or periodontal therapy—are needed. A collaborative treatment plan outlines the steps, responsibilities, and realistic expectations for healing and restoration.
The treatment timeline can include diagnostic imaging, surgical placement of the implant, a period for the implant to integrate with bone, and final restorative stages when the prosthesis is attached. Throughout this process, the team explains what to expect at each phase so patients can make informed decisions and prepare for recovery and follow-up care.
Patients who choose implant restorations benefit from a solution that emphasizes function, esthetics, and preservation of oral structures. If you are considering tooth replacement options, a personalized consultation will clarify your suitability for implants and describe the individualized plan that best meets your goals and clinical needs.
At The Haddon Dentist, we focus on predictable, patient-centered implant restorations that combine sound biology with refined prosthetic design. If you’d like to learn more about how implant-supported restorations could restore your smile and oral function, please contact us for additional information and to schedule a consultation.

Implant restorations replace a missing tooth from root to crown using a biocompatible post, an abutment, and a visible prosthesis such as a crown, bridge, or denture. The post is placed in the jawbone where it serves as an artificial root and, once integrated with bone, provides a stable foundation for the restoration. Precision in the fit and design of the abutment and prosthesis ensures the restoration replicates the form and function of a natural tooth.
The biological process called osseointegration anchors the implant in bone and is essential to long-term success. Because the implant transmits chewing forces into the jaw, it helps preserve bone volume and supports surrounding teeth. This combination of surgical and prosthetic steps allows the restoration to perform like a natural tooth in daily function and appearance.
Implant restorations offer enhanced stability and function compared with removable dentures and often preserve more of the adjacent natural teeth than traditional bridges. By replacing the root as well as the crown, implants transmit forces through the bone and help maintain facial structure and jaw health. Many patients experience improved comfort for chewing and clearer speech because the prosthesis is anchored rather than resting on gums or relying on neighboring teeth.
From an oral health perspective, implants reduce the need to alter healthy adjacent teeth and help prevent the bone loss that commonly follows tooth extraction. Well-designed implant restorations also simplify hygiene in many cases because contacts and emergence profiles are shaped to resist food trapping. Together these benefits support long-term function and predictable esthetic results when cases are planned and executed carefully.
Implant posts are commonly made from titanium or titanium alloys because of their proven biocompatibility and strength, while visible restorations are fabricated from high-strength ceramics, zirconia, or porcelain-fused materials depending on functional and esthetic needs. Monolithic ceramic restorations offer strength and minimal layering, whereas layered ceramics can provide enhanced translucency for highly esthetic zones. Abutments may be titanium, zirconia, or custom-angled components chosen to support the emergence profile and soft-tissue contours.
Design considerations such as crown shape, contact points, and occlusal scheme are tailored to distribute bite forces evenly and to protect both the prosthesis and surrounding tissues. Digital workflows, including intraoral scanning and CAD/CAM milling, improve fit and shade matching and often reduce adjustment time at delivery. These material and design choices are selected to balance durability, esthetics, and ease of maintenance for each patient.
Candidacy for implant restorations is determined by a combination of oral health, bone quantity and quality, and general medical factors that can influence healing. Good oral hygiene and controlled periodontal health are important prerequisites, and sufficient jawbone is needed to support an implant unless preparatory grafting is planned. Certain systemic conditions, tobacco use, and medications can affect outcomes, so a thorough medical and dental history is reviewed during evaluation.
Many patients who initially lack adequate bone can become candidates after targeted procedures such as bone grafting or sinus augmentation, and treatment plans are individualized to account for those needs. A consultation with imaging and clinical examination clarifies whether a single implant, multiple implants, or an implant-supported prosthesis is the most predictable option. The goal is a treatment pathway that prioritizes long-term stability and function.
Treatment begins with a comprehensive evaluation that includes clinical examination and diagnostic imaging to map bone anatomy and plan implant position relative to the planned restoration. Surgical placement of the implant is followed by a healing phase during which osseointegration occurs; this period commonly lasts a few months but can vary based on the implant site and any adjunctive procedures. In some cases, immediate or early loading protocols can be used when primary stability and other factors make it appropriate.
After adequate integration, an abutment is attached and the final prosthesis is fabricated and delivered, often using digital design and milling to enhance precision. Maintenance appointments and occlusal checks follow delivery to ensure the restoration is functioning as intended. Your clinician will outline a personalized timeline so you understand each phase and expected healing milestones.
Accurate surgical placement establishes the foundation for prosthetic success by positioning the implant at the correct depth and angulation to support the final restoration and surrounding soft tissues. Achieving primary stability at placement and minimizing micromovement during healing are important for predictable osseointegration. Surgical planning often uses 3D imaging and surgical guides to translate the restorative plan into precise implant positioning.
Biologic integration of bone to the implant surface is influenced by factors such as bone quality, surgical technique, and postoperative care, and it is critical to long-term function. Properly integrated implants distribute occlusal forces efficiently and reduce the risk of mechanical complications, while poor integration can lead to mobility and failure. Close monitoring during the healing phase and adherence to postoperative instructions improve the likelihood of lasting success.
For a single missing tooth, an implant-supported crown restores both appearance and function without altering neighboring teeth, while multiple adjacent missing teeth may be rehabilitated with an implant-supported bridge. For full-arch replacement, implant-retained overdentures and fixed solutions such as All-on-4® or All-on-6® concepts provide options that vary in maintenance, stability, and restoration type. The choice between a removable overdenture and a fixed prosthesis depends on anatomy, hygiene capability, and the patient’s restorative goals.
Each prosthetic option has distinct advantages and maintenance requirements, and the restorative team evaluates bone anatomy, esthetic demands, and occlusal function when recommending a solution. Custom abutments and prosthesis designs are used to achieve optimal emergence profiles and soft-tissue support. Collaborative planning with the surgical team ensures the selected prosthesis can be supported predictably over the long term.
Daily home care is essential: brush carefully around the restoration, clean interproximally with floss or interdental brushes designed for implants, and avoid habits that place undue stress on the restoration such as biting very hard objects. Consistent, gentle plaque control around implant margins reduces the risk of inflammation and peri-implant disease. Using nonabrasive toothpaste and instruments recommended by your clinician helps protect the prosthetic surfaces and surrounding tissues.
Professional maintenance visits allow your dental team to evaluate soft tissue health, assess occlusion, and tighten or adjust prosthetic components as needed. Regular monitoring also facilitates early detection of wear, screw loosening, or biological changes that can be managed conservatively. With attentive home care and scheduled professional oversight, implant restorations can provide reliable function for many years.
Complications can be biological, such as peri-implant mucositis or peri-implantitis, or mechanical, such as screw loosening, fracture of the prosthesis, or wear of restorative materials. Early signs include redness, bleeding on probing, changes in fit, or persistent discomfort, and prompt evaluation allows targeted interventions. Management may range from improved hygiene and non-surgical therapy to surgical intervention or prosthetic repair depending on severity.
Mechanical issues are often addressed by tightening or replacing components and by adjusting occlusion to reduce excessive forces, while biological problems may require debridement, antimicrobial measures, or regenerative procedures in collaboration with specialists. A preventive maintenance program and timely attention to symptoms are the best strategies to limit complication severity and preserve the restoration.
Begin with a consultation where clinical findings and digital imaging are used to determine suitability and to outline a personalized treatment plan, including any preparatory procedures that may be needed. During this visit the prosthodontist-led team reviews restorative goals, explains the sequence of surgical and prosthetic steps, and discusses how modern digital workflows can streamline treatment. Clear communication about expectations and a thorough exam help patients make informed decisions about care.
To schedule a consultation or to learn more about implant options, call New Patients at (856) 281-1356 or request an appointment through the office contact avenues listed on our site. The Haddon Dentist emphasizes collaborative planning and evidence-based techniques to deliver predictable, esthetic implant restorations tailored to each patient’s needs.

The path to a restored, high-functioning smile is a journey of precision, and it begins with a single, focused conversation. We invite you to experience the intersection of clinical mastery and uncompromising luxury at The Haddon Dentist. Whether you are seeking the immediate results of CEREC® same-day crowns, exploring the life-changing benefits of dental implants, or ready to revitalize your aesthetic with professional teeth whitening, we are here to curate a plan tailored exclusively to you. Your time is your most valuable asset, and we cherish the opportunity to provide the elite care you deserve in an environment that respects your comfort and your goals.